DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
RECOGNITION AND ASSESSMENT
- Use this guideline only in patients where the most likely diagnosis is acute myocardial infarction
- To check you are using the correct guideline, use Assessment of chest pain suspected to be cardiac in origin guideline
Symptoms and signs
- Severe, persistent chest pain
- Dyspnoea
- Fear
- Pallor
- Sweating
- Anxiety
- Peripheral vasoconstriction
- Shock
Investigations
- ECG (see below)
- Locally available cardiac biomarkers of myocardial injury
- Raised cardiac biomarkers signify myocardial infarction, not unstable angina
- A raised troponin I concentration can suggest myocardial necrosis but can also occur in a number of other conditions:
- auto-immune disease
- congestive cardiac failure
- critical illness
- dilated cardiomyopathy
- extreme physical effort
- hypertension
- hypothyroidism
- multiple injury
- myocarditis
- pericarditis
- pneumonia
- pulmonary embolism
- renal failure
- sepsis/septic shock
- subarachnoid haemorrhage
- tachyarrythmias
- vasculitis
- Plasma cholesterol profile (within 12 hr of onset of symptoms; otherwise leave for at least 6 weeks)
- Venous blood glucose and HbA1c
- FBC, INR, APTT
IMMEDIATE TREATMENT
- Aspirin 300 mg (chew and swallow)
- Diamorphine 1 mg/min IV until pain relieved, up to maximum 10 mg (5 mg in elderly or frail patients)
- Metoclopramide 10 mg IV over 1-2 min (5 mg <60 kg) with ≥8 hr before repeating
- Oxygen - see Hypoxaemia guideline
- Bisoprolol 2.5 mg oral daily, unless contraindicated (e.g. decompensated heart failure, bradycardia)
- Unless history of CKD present, atorvastatin 80 mg once daily for all acute coronary syndromes. If history of CK, start with atorvastatin 20 mg once daily
Admission
- Admit all patients with acute myocardial infarction (MI), or unstable angina with acute ST depression and/or raised troponin I to CCU under the care of duty consultant cardiologist. Contact on-call cardiology SpR immediately for immediate transfer and treatment
- If ECG shows ST elevation MI (STEMI), follow Management of STEMI below
- ≥2.5 mm in men aged <40 yr
- ≥2 mm in men aged ≥40 yr
- ≥1.5 mm in women regardless of age
- If patient has a Non-ST elevation MI (NSTEMI), follow Management of NSTEMI below
MANAGEMENT OF STEMI
- Administer loading dose of aspirin (300 mg oral) if not already given
- Immediately administer prasugrel (contraindicated in stroke/TIA) and not taking oral anticoagulant
- if aged <75 yr, weight <60 kg, then load with 60 mg and then 5 mg daily for 1 yr
- if aged <75 yr, weight >60 kg, then load with 60 mg and then 10 mg daily for 1 yr
- if aged ≥75 yr, then load with 60 mg and then 5 mg daily for 1 yr
- if prasugrel not suitable (stroke/TIA or aged ≥75 yr and increased risk of bleeding) use clopidogrel 600 mg oral (unlicensed loading dose)
- Refer to cardiology for primary angioplasty (pPCI), the national default strategy for STEMI management
- If transportation time to a pPCI ready hospital is likely to be >2 hr, then consider thrombolysis, and follow Thrombolytic therapy (STEMI), and immediate transportation to a pPCI centre thereafter
- if decision is not for primary angioplasty, only give thrombolytic therapy if directed by on-call cardiology service - then follow Thrombolytic therapy (STEMI) guideline. Usually, a contraindication for primary angioplasty is a contraindication for thrombolysis
MANAGEMENT OF NSTEMI
- Treatment of choice for most patients for NSTEMI is early (within 72 hr) inpatient cardiac catheterisation with early revascularisation, either by percutaneous intervention (PCI) or coronary artery bypass graft (CABG)
- patients unlikely to be suitable for an early invasive strategy because of frailty or multiple comorbidities should have that decision made early and by an experienced clinician
- Prescribe fondaparinux 2.5 mg once daily by SC injection
- Antiplatelet therapy has changed since 2020
- If patient has an NSTEMI, but is likely to go through an invasive angiographic assessment early, then aspirin alone is administered
- Dual antiplatelet therapy decisions will be made in the catheter laboratory
- If an invasive strategy may be delayed then give clopidogrel loading dose 600 mg oral and 75 mg daily
- Risk of bleeding is increased in patients with low body weight (<50 kg), physiological frailty, severe liver (bilirubin >2 x upper limit of normal and AST/ALT/alk phos >3 x upper limit of normal) or renal failure (eGFR <20 mL/min, or serum creatinine ≥ 200µmol/L), alcohol abuse, thrombocytopenia or defective platelet function or impaired clotting, anaemia and following surgery, trauma or haemorrhagic stroke
- seek advice from appropriate team (e.g. cardiology, renal, liver or haematology)
NON-DIABETIC PATIENTS WITH BLOOD GLUCOSE >11 MMOL/L AND ALL PATIENTS WITH DIABETES MELLITUS
- On admission, check blood glucose/HbA1c and, if blood glucose is >11 mmol/L, commence variable rate insulin infusion (VRII) - see Hyperglycaemia: can’t eat/drink guideline. In patients with diabetes/raised blood glucose, seek advice from endocrinologist/diabetes nurse specialist early
SUBSEQUENT MANAGEMENT
- Aspirin 75 mg oral daily (to be continued indefinitely) plus:
- if STEMI and treated by pPCI with no history of CVA or TIA, then either prasugrel or clopidogrel may be appropriate
- otherwise clopidogrel 75 mg oral daily for 1 yr
- For prasugrel
- if aged <75 yr, weight <60 kg, then maintenance dose 5 mg daily for 1 yr
- if aged <75 yr, weight >60 kg, then maintenance dose 10 mg daily for 1 yr
- if aged >75 yr, then maintenance dose 5 mg daily for 1 yr
- Bisoprolol 2.5 mg oral daily, or atenolol 25 mg 12-hrly (to be titrated to target heart rate of 60 bpm and continued indefinitely)
- If no clinical suspicion of significant mitral/aortic stenosis or hypertrophic cardiomyopathy, plasma creatinine <300 μmol/L and there is no other contraindication to using ACE inhibitor, start ramipril - see Ramipril guideline. Check electrolytes on day 3-5. Increase titration rapidly to achieve a dose on discharge as near to 10 mg as achievable
- Check statin (atorvastatin 80mg) has been prescribed, target LDL to ≤2.0 mmol/L or non-HDL cholesterol to ≤2.6 mmol/L, subject to renal function (see above)
- give patient information sheet
- If pain persists, consider glyceryl trinitrate (GTN) infusion - see Glyceryl trinitrate guideline or further dose of atenolol 5 mg IV if heart rate >70 bpm and systolic BP >100 mmHg
- If pain persists, contact duty cardiology team to facilitate transfer to ward/CCU
- Unless complications ensue, recommend early return to physical activity:
- mobilisation depends on revascularisation strategy, with early mobilisation and discharge by day 3 the norm post STEMI managed with an early invasive strategy
- Refer all patients to rehabilitation co-ordinator, who will arrange for assessment of all suitable patients by cardiac rehabilitation team as soon as practically possible after discharge
- patients not wishing to join rehabilitation programme - provide appropriate dietary advice
- Refer all patients treated with glucose and insulin infusions to diabetes nurse specialist to distinguish diabetes from stress-induced hyperglycaemia
MONITORING TREATMENT
- Continuous ECG monitoring for 24-48 hr (longer if continuing instability or arrhythmia)
- Measure BP 4-hrly for 24 hr, then twice daily
- Daily 12-lead ECG. Plasma troponin I next day, as peak troponin indicates infarct size
- Observe for specific complications (more likely to occur if patient not re-perfused)
Specific complications
- In all complications, seek further cardiological input
Arrhythmias
Pericarditis
- More likely after large or late presenting infarcts
- Positional pain with persistent/intermittent pericardial rub 2-5 days after infarction
- Adequate analgesia (may need diamorphine). Give colchicine 500 microgram 12-hrly (500 mg once daily <70 kg) (unlicensed) if no contraindication
Recurrent ischaemic pain
- Isosorbide mononitrate SR oral (GTN infusion if necessary - see Glyceryl trinitrate guideline
- If persistent chest pain occurs, refer to duty cardiology team for consideration of inpatient stress testing, coronary angiography and possible inpatient revascularisation
- If re-infarction occurs during admission, contact duty cardiology team immediately
Cardiac failure
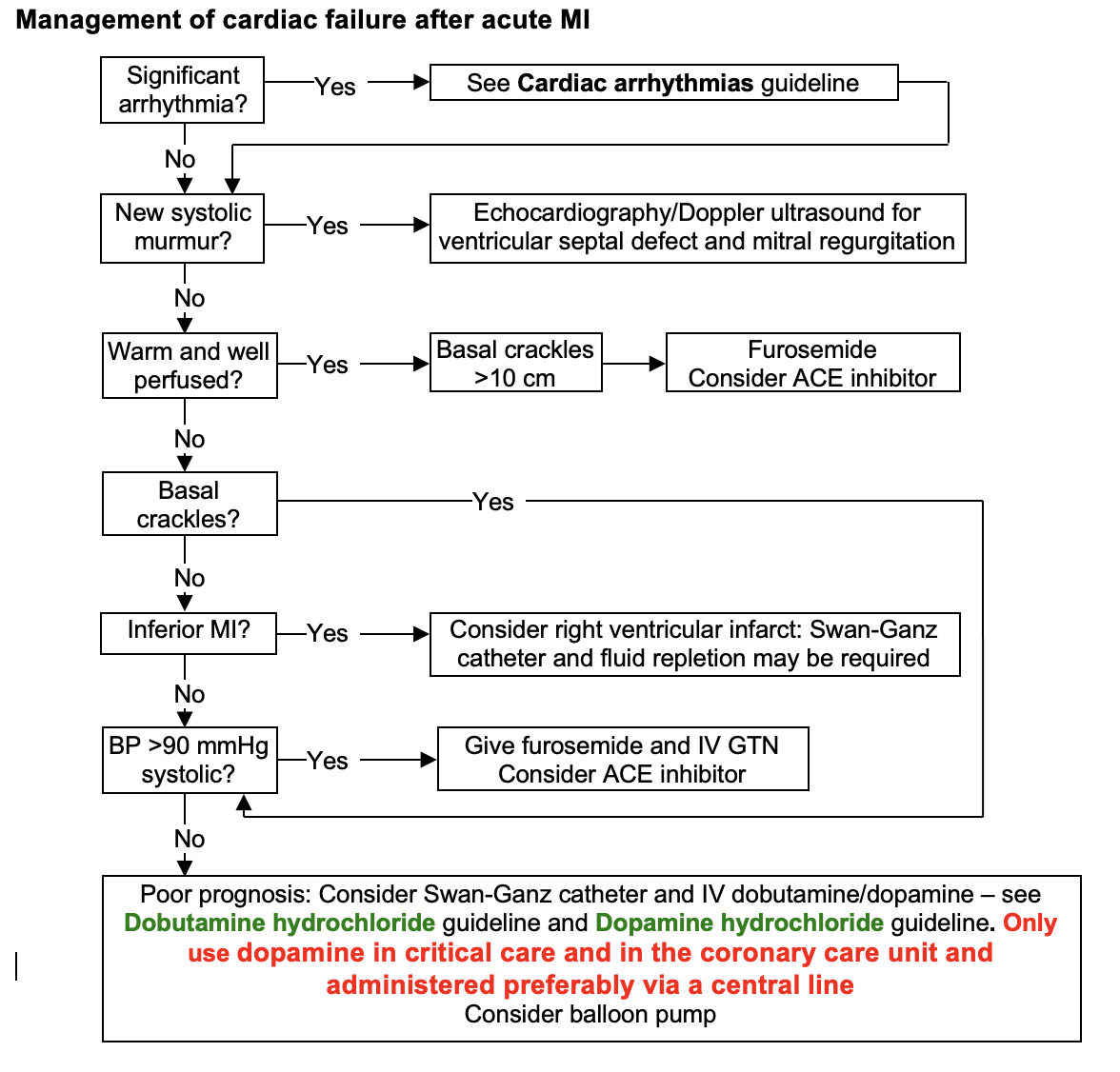
- In patients with left ventricular failure (LVF) or impaired LV function, introduce an ACE inhibitor as soon as this is practical - see Acute heart failure guideline
- In patients with significant LVF and/or anterior infarct, arrange echocardiogram as inpatient, to document LV function and exclude LV aneurysm and/or thrombus
DISCHARGE AND FOLLOW-UP
- If no complications, discharge home on day 3 (72 hr post admission)
- Check risk factors for recurrent MI (e.g. smoking, hyperlipidaemia, hypertension, obesity) and advise or treat accordingly (mortality in first 2 years is doubled in those who continue to smoke and is 3.5-times greater if total cholesterol >6.5 mmol/L)
- Explain graded return to full activity (see advice booklet)
- Where appropriate, ensure patient has climbed stairs to assess for chest pain/shortness of breath
- Ensure advice booklet and chest pain alert card have been issued
- If taking atorvastatin, ensure GP letter regarding intensive statin therapy accompanies patient on discharge
- Warn about post-infarct angina
- Ensure GTN 400 microgram spray for sublingual use has been prescribed TTO and patient has been counselled on use
- Advise not to drive as per DVLA rules and check with insurer (Group 2 drivers must notify DVLA, taxi drivers must notify local council)
- Ensure referral has been made to cardiac rehabilitation team
- Check that rehabilitation plan has been made
- middle grade in cardiology will be able to review patients who attend as an outpatient at cardiac rehabilitation. Rehabilitation co-ordinator will arrange
- if patient declines cardiac rehabilitation or is unsuitable for programme, refer to cardiology follow-up clinic
- Check that follow-up has been arranged in diabetic clinic for all patients treated with glucose and insulin infusions
Follow-up clinic visit
- Ask about smoking, exercise and weight reduction
- Ask about angina - if occurring, consider referral for further cardiology assessment
- Look for signs of heart failure and measure BP
- Check cholesterol (target LDL to ≤2.0 mmol/L or non-HDL cholesterol to ≤2.6 mmol/L)
- If patient has not been to catheter laboratory, consider treadmill exercise if symptomatic
- Encourage return to work 1 month after infarction
- Resume driving 1 month after infarction (except Group 2 drivers), unless qualifies for a 1 week DVLA driving ban (normal LV function, single vessel disease, treated by PCI)
- Unless there are contraindications, all patients should be taking the following treatment
STEMI
- ACE inhibitor (target dose ramipril 10 mg or equivalent)
- Statin therapy (target dose atorvastatin 80 mg or equivalent, target LDL to ≤2.0 mmol/L or non-HDL cholesterol to ≤2.6 mmol/L,unless history of CKD)
- Beta-blocker (target dose to achieve heart rate of 60 bpm at rest)
- Aspirin (75 mg) indefinitely
- If STEMI and treated by PCI, prasugrel or clopidogrel 75 mg oral daily for 1 yr, as per cardiac catheter laboratory instruction. Prasugrel maintenance dose guided by weight and age (5 or 10 mg daily)
NSTEMI
- ACE inhibitor (target dose ramipril 10 mg or equivalent)
- Statin therapy (target dose atorvastatin 80 mg or equivalent, unless history of CKD)
- Beta-blocker (target dose to achieve heart rate of 60 bpm at rest)
- Antiplatelet therapy aspirin (75 mg) indefinitely, prasugrel or clopidogrel 75 mg oral daily for 1 yr, as per cardiology instruction. Prasugrel maintenance dose guided by weight and age (5 or 10 mg daily)
Last reviewed: 2024-03-25