DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
Table 1: Substance misuse contact numbers
| Royal Stoke alcohol liaison nurses (ALN) | Stoke community drug and alcohol service |
Staffordshire services |
| Ward pager: 07623 676286 | 01782 283113 | Edward Myers Unit: 01782 441715 |
| A&E pager: 07623 611822 | Leek: 01538 384361 | |
| Office: 01782 672703 | Newcastle: 01782 637658 | |
| Referrals on OrderComms | Stafford/south of county: 01785 270080 | |
| Weekends: HALT 01782 637658 |
RECOGNITION AND ASSESSMENT
- Alcohol withdrawal can be a presenting feature or occur as an unexplained development in a patient who has been admitted for other reasons and deprived of alcohol. Untreated, it carries a 15% mortality rate. Mild withdrawal generally begins 6-8 hr after last drink, but can be sooner or considerably delayed. Moderate-severe withdrawal occurs about 48 hr after last drink. Pay particular attention if frequent attendance at hospital (e.g. upper GI symptoms)
Symptoms and signs
- Anxiety
- Sweating
- Tremor
- Ataxia
- Confusion
- Assess severity with Clinical Institute Withdrawal Assessment of Alcohol Scale (revised CIWA-Ar) form . Ask specific questions shown for each category and use CIWA-Ar form to derive score from answers or observations
- scores <10: do not need medication for withdrawal
- scores ≥10: will need benzodiazepines for symptom control as in IMMEDIATE MANAGEMENT section below
- For advice on assessment, contact alcohol liaison nurse (see Table 1 for contact numbers)
- Patients who attend intoxicated but have a high degree of tolerance towards alcohol are at risk of developing alcohol withdrawal symptoms even while their alcohol level may still seem high
Alcohol history
- Complete Alcohol consumption screening tool (AUDIT C)
- Quantity, frequency and highest daily alcohol use
- Previous treatment for alcohol misuse
- Previous abstinence
- Triggers for drinking
- Psychiatric problems
- Motivation
Routine investigations
- If decompensated alcoholic liver disease (ascites, encephalopathy) or a GI bleed, blood cultures
- FBC
- U&E
- LFT
- INR
- Bone profile plus magnesium and phosphate
- Blood glucose
Optional investigations
- Arterial blood gases (severe withdrawal or severe systemic upset)
- If illicit drug use suspected, urine drugs of abuse screen. Some of the newer drugs ('legal highs') may be difficult to identify
- Breath/blood alcohol
- Gamma-glutamyl transpeptidase test (GGT)
Differential diagnosis
- See Delirium (acute confusional state) in older people guideline
- Decompensated Liver Disease with hepatic encephalopathy
- Withdrawal of intoxication with drug(s) of misuse. See Withdrawal of drug(s) of dependence guideline
Alcohol related brain damage (ARBD)
- If patient presents to ED appearing intoxicated, confused, 'off legs', consider ARBD
- Alcohol related brain damage (ARBD) is an umbrella term used to describe a spectrum of brain disorders that include alcohol related dementia, alcohol amnesic syndrome and Wernicke’s-Korsakoff's syndrome.
- if left untreated can lead to irreversible brain damage, disorders of the nervous system and death
- Diagnosis is supported by the presence of the following:
- alcohol related hepatic, pancreatic, gastro-intestinal, cardiovascular or renal damage
- ataxia or peripheral neuropathy
- evidence on neuro imaging of brain atrophy
UHNM admission criteria
- Confusion or hallucinations
- Epilepsy or history of fits
- Undernourished
- Severe vomiting or diarrhoea
- Uncontrollable withdrawal symptoms
- Acute physical illness requiring admission
- Decompensated liver disease
If patient does not meet criteria for admission but shows signs of, or is at risk of alcohol withdrawal
- Advise patient to avoid sudden reduction in alcohol intake
- Refer to alcohol liaison team or give information on local alcohol support services
- Give a dose of Pabrinex IV as per guidance. If the patient remains in the department for observational purposes, continue with Pabrinex IV 8-hrly as per guideline
IMMEDIATE MANAGEMENT
Alcohol withdrawal assessment (based on CIWA-Ar scale) and symptom control
- Assess vital signs and record on NEWS chart (review alongside CIWA-Ar assessments)
- Complete assessment using CIWA-Ar scale
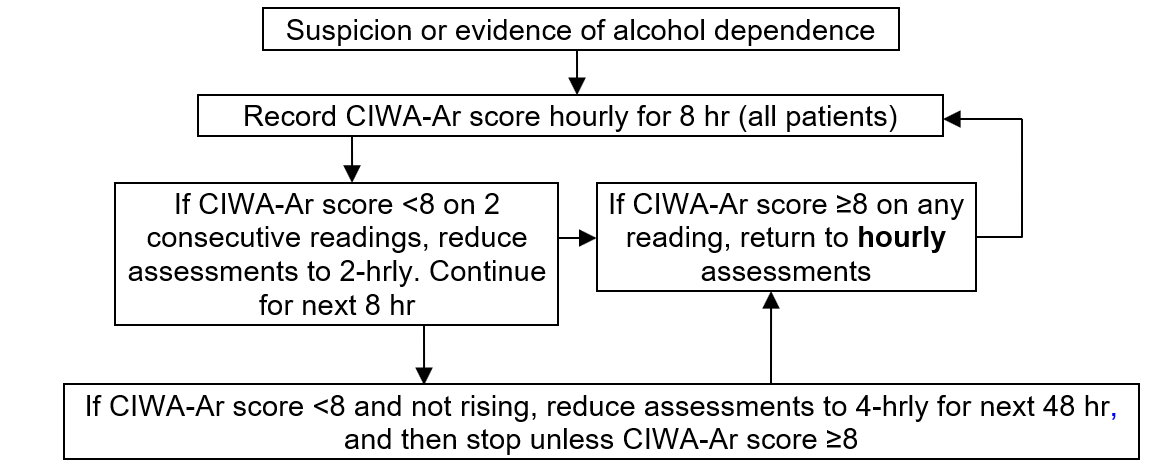
- See CIWA-Ar Flowchart below for assessment guidance
- If CIWA-Ar score ≥10, commence symptom triggered treatment with oral benzodiazepines
- Prescribe diazepam unless patient is frail elderly, unable to tolerate diazepam, showing signs of delirium tremens, has respiratory failure or severe liver impairment (e.g. INR >2 and bilirubin >200 or hepatic encephalopathy) in which case use lorazepam
- Administer as required medication as directed by CIWA-Ar assessments and record doses given on drug chart and CIWA-Ar chart
- If patient scores 11-12 on AUDIT-C or requires CIWA-Ar monitoring, refer to alcohol liaison team
- If patient usually on a regular benzodiazepine e.g. temazepam 10 mg at night, continue this with additional diazepam or lorazepam prescribed as required to manage alcohol withdrawal symptoms
Alcohol withdrawal in pregnancy
- Commence CIWA-Ar symptom assessment and discuss with alcohol liaison team, substance misuse midwife and Edward Myers Unit regarding tapered reduction of benzodiazepines
The aim is to prevent features of withdrawal without over sedation. Individual dose requirements vary considerably and can be decided only by assessing response regularly and omitting or adding doses as necessary. Lorazepam and diazepam normally given orally
CIWA-Ar flowchart
| CIWA-Ar score | Medication |
| <10 | Nil |
| 10-15 | 5 mg diazepam or 0.5 mg lorazepam |
| ≥16 | 10 mg diazepam or 1 mg lorazepam |
Note: Some patients may require higher than BNF recommended limits of benzodiazepines if severe withdrawal symptoms
Case discussion with senior medical staff is appropriate if:
- Patient has required 3 mg lorazepam or 30 mg diazepam over 3 hr
- CIWA-Ar score >35
- Evidence of Delirium Tremens (which should be viewed as a medical emergency)
Possible actions for discussion
- Reassess patient - check conscious levels, respiratory status and alcohol withdrawal symptoms, and look for any evidence of other organic pathology
- If withdrawal symptoms persist, consider changing from diazepam to lorazepam
- If unable to tolerate oral benzodiazepines or symptoms of severe hallucinations or agitation, consider use of parenteral lorazepam 1 mg (preferably IV into a large vein) with interval between doses of at least 15 min (IV) and 30 min (IM)
- Do not use IM route in patients with bleeding/clotting disorders
- Haloperidol 1-5 mg can be added to enhance sedative effects of benzodiazepines (see BNF for contraindications)
- If total dose of lorazepam has reached 8 mg and patient still agitated - discuss with critical care
Other indications for discussion with critical care
- Respiratory depression
- Patient in state of extreme agitation
Fluids and electrolytes
- Monitor and replace electrolytes, magnesium and phosphate and give adequate hydration see Fluid management guideline
- defer glucose infusions until after first dose of Pabrinex given as it can precipitate Wernicke’s encephalopathy
Vitamin therapy
- Most effective when given parenterally as oral absorption is poor; IV route is preferable but if this is not available, use IM route
All patients
- Give parenteral thiamine as Pabrinex IV high potency injection 2 pairs of ampoules (mixed) by IV infusion in sodium chloride 0.9% 100 mL over 30 min 8-hrly
- if IV route not available, give 1 pair of ampoules deep IM into gluteal muscle 12-hrly. Use Pabrinex preparation specific to IM injections
- Patients with decompensated liver disease, malnourishment or significant weight loss or memory disturbance are at risk of Wernicke’s encephalopathy, continue Pabrinex for 72 hr at frequency stated above
- In all other patients 72 hr of Pabrinex is not essential e.g. if patient is considered medically fit for discharge within this time it does not need to be continued
- If Wernicke’s encephalopathy is suspected or confirmed and physical symptoms persist beyond 72 hr but patient is improving symptomatically, give 1 pair of ampoules IV or deep IM once daily for as long as symptoms continue to improve and for a minimum of 5 days in total
- Prescribe oral thiamine 100 mg 8-hrly for all patients on discharge and advise GP via discharge letter to continue this for 3 months in the community
- Note vitamin B Compound strong tablets are not indicated in alcohol dependent patients. Do not discharge patients on vitamin B compound and ensure it is stopped in those admitted on vitamin B solely for the reason of alcohol dependency unless malnourished
- If patient malnourished refer to dietitian and discuss need for ongoing vitamin supplementation
MONITORING THERAPY
- If drowsy, confused or there is concern about previous readings, blood glucose 2-hrly
SUBSEQUENT MANAGEMENT
Seizures
- Manage seizures, see Seizure guideline and Cluster seizures guideline. However, withdrawal seizures alone do not signify epilepsy and maintenance anticonvulsant therapy is unnecessary
DISCHARGE AND FOLLOW-UP
- Where possible liaise with alcohol liaison nurses to plan discharge
- Ensure all patients have been assessed for alcohol dependency with the AUDIT alcohol screening tool
- Alcohol liaison team may advise prescribing Acamprosate:
- body weight ≥60 kg - 666 mg 8-hrly
- body weight <60 kg - 666 mg at breakfast, 333 mg at midday and 333 mg at night
- to be continued on discharge and reviewed by GP or community alcohol service
Further community support
- Refer patients living in Stoke-on-Trent to Stoke community drug and alcohol service, refer patients living in the rest of Staffordshire to One Recovery - see Table 1 for contact numbers
Screening results (AUDIT score)
- <8: no action required
- 8-19: advice and offer referral to community alcohol services
- 20+: refer to alcohol liaison nurse (see Table 1 for contact numbers)
Supported home detoxification (Royal Stoke only)
- Patients assessed by a consultant as medically fit for discharge, who have received in-patient detoxification for ≥72 hr, but still have CIWA-Ar scores ≥8, may be suitable for continued home detoxification
- This service is only available to those assessed by alcohol liaison nurses and deemed suitable
- Detoxification will be supervised and patients given appropriate follow-on support
- Generate discharge letter for GP and advise any alcohol intervention and follow-up requirements
Additional advice on discharge
- Advise patient to contact the DVLA and car insurance provider, and that with alcohol related illness they should not drive for 6 months; with alcohol withdrawal they should not drive for 12 months
Last reviewed: 2024-04-10