DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
Would a venous blood gas give the required information?
INDICATIONS
- Moderate or severe respiratory failure
- Patients with severe respiratory or cardiac disease scheduled for major abdominal or thoracic surgery
- Suspected acid-base disturbance
- Suspected carbon monoxide poisoning
- Emergency blood sampling when venepuncture impossible
CONTRAINDICATIONS
- Consider risks and benefits in patients with bleeding diathesis
WHICH ARTERY?
Radial Artery
Position of patient
- Arm extended and supported on pillow with wrist extended 20°
Angle of needle to skin
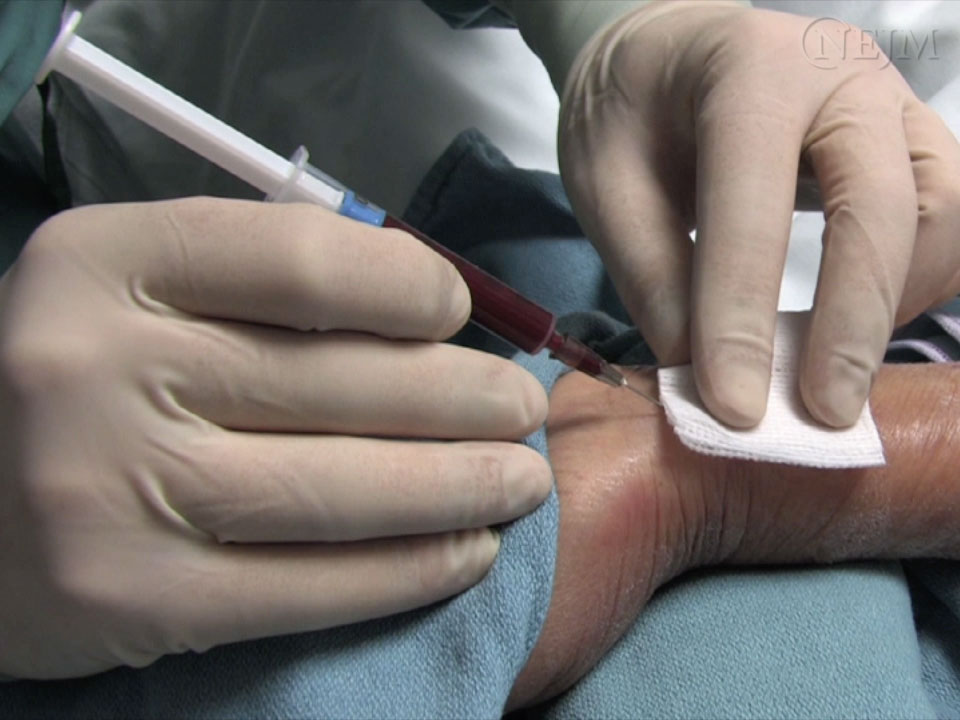
- 30°. See Figure 1
Puncture site
- Proximal to proximal transverse crease on radial aspect of wrist
Advantages
- Easily accessible
- Easily compressible, therefore useful if there is known bleeding tendency
Contraindications
- Buerger's disease
- Raynaud's disease
- Arteriovenous dialysis shunt present or imminent
- Absent ulnar collateral circulation - relative contraindication, consider Allen's test
Brachial artery
Position of patient
- Arm extended and supported on pillow
Angle of needle to skin
- 30°
Puncture site
- Medial to biceps tendon in antecubital fossa
- CARE: Median nerve medial
Advantages
- Easily accessible
Disadvantages
- Risk of ischaemia
Contraindications
- Arteriovenous fistula in arm
- Elbow fractures
Femoral artery
Position of patient
- Supine
Angle of needle to skin
- 60°
Puncture site
- Mid-inguinal point 2 cm below inguinal ligament
- CARE: Femoral nerve lateral and femoral vein medial
Advantages
- May be only quickly accessible artery in shocked patient
Disadvantages
- Risk of infection and ischaemia
- Venous sample more likely than at other sites
Contraindications
- Severe peripheral vascular disease
- Aortofemoral bypass surgery
EQUIPMENT
- Non-sterile disposable gloves
- Alcohol wipes or other antiseptic solution
- Lidocaine 1% plain 2 mL, 25 or 27 G needle and/or ice pack
- Blood gas syringe with 23 G needle
- smaller needles have shown longer draw times, and no pain benefit
- Plastic syringe cap
- Cotton wool balls or similar to press over site after arterial puncture
- Sharps' Bin
PROCEDURE
- If not competent in procedure, organise supervision by a clinician experienced in the procedure
Consent
- Explain procedure and reassure patient
- Obtain and record consent
- Positive Patient Identification (PPID) confirmed
Preparation
- If blood gas analysis not going to be performed within a few minutes, have an ice bag ready to cool sample
- Consider using ice (in a plastic bag) on skin for up to 3 min or cryogesic spray for additional/alternative analgesia to lidocaine
- Check concentration of oxygen patient is breathing at time arterial sample is taken
- if time permits, check it remains constant for 15 min before sampling
- note it on request form, in patient notes and on results printout
- Note patient's temperature on request form
Aseptic technique and position of patient
- Select site of puncture and position patient. See Which artery
- Wear gloves, cleanse patient's skin
Local anaesthetic
- Palpate artery and infiltrate skin with lidocaine plain 1% 0.5-1 mL
- always aspirate before injection of local anaesthetic to prevent injection of lidocaine into the artery
Sampling
- Hold blood gas syringe with 23 G needle, bevel up; for radial (Figure 1) and brachial arteries at about 30° to skin surface; for femoral artery at 60°
- Advance needle towards artery
- with some blood gas syringes, blood pulsates into syringe; others will need to be drawn
- if shooting pain felt, nerve may have been entered. Remove needle and redirect
- if no blood obtained, withdraw needle slowly, observing for pulsation at base of needle; arterial blood often enters during withdrawal
- if necessary, try once more. If unsuccessful, seek help
- Obtain 1.5-2 mL blood
- a smaller volume may suffice for immediate analysis
- Withdraw needle
- Apply pressure to site for 5 min, or if site bleeds, longer
- Dispose of needle in sharps bin
- Remove bubbles in syringe by holding hub upwards and gently tapping side and depressing plunger
- Immediately cap syringe and gently mix for 30 sec
- Attach patient ID label to sample and record FiO2 (%), patient temperature and time sample taken
- If source of blood (arterial/venous) uncertain, take heparinised venous sample for comparison
SPECIMEN
- Take sample to nearest blood gas analyser for analysis
- ensure all data fields displayed on screen are accurately completed
- Try to ensure sample is analysed within 15 min of drawing
- Clotting increases as sample ages, therefore ensure syringe is continuously and gently mixed to reduce risk of clotting
- Do not analyse aged samples (taken >20 min before)
- Ensure printed record displays all inputted details
Last reviewed: 2023-12-06