DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
RISK FACTORS
- Constipation likely in patients who are:
- immobile/less mobile than usual
- drinking less fluid than usual
- eating less cereal, fruit and vegetables than usual
- taking prescribed opioid type medication, e.g. codeine and/or iron or post-operatively
- If taking opioids, prescribe laxatives routinely
ROUTINE BOWEL CARE
- Enquire about usual bowel habit
- If patient from nursing/residential home and unable to provide information, request the Home-to-Hospital form
- Enquire about laxatives from GP or bought over the counter
- Enquire about adverse effects from laxatives in the past
Routine nursing care
- Complete bowels section on nursing sheets daily
- Encourage fluids (≥1 L/day)
- if patient is on restricted fluids for heart failure, may have to avoid giving >1 L/ day
- If patient usually takes laxatives at home, prescribe in hospital unless there are now contraindications
Toileting
- Ensure toileting facilities safeguard privacy and dignity
- Transfer to toilet, if possible
- Avoid commode
- Prevent inhibition
- Ensure privacy
- Control noise (try to locate toilets in quieter part of ward)
- Ensure patient can easily summon help
- make bell or button accessible and respond promptly
- Control odours (use air freshener if necessary)
BOWELS NOT OPEN FOR 3 DAYS = CONSTIPATION
Cautions
- In patients with suspected intestinal obstruction, ask for senior advice
- take care when using laxatives of any kind
- If haemorrhoids or anal fissure, avoid rectal preparations
- In patients with inflammatory bowel disease, colitis or Crohn’s disease, avoid macrogols
Perform digital rectal examination
- Document findings
- If rectum full of faeces, follow Faecal impaction below
- If rectum empty, follow Bowel transit disorder below
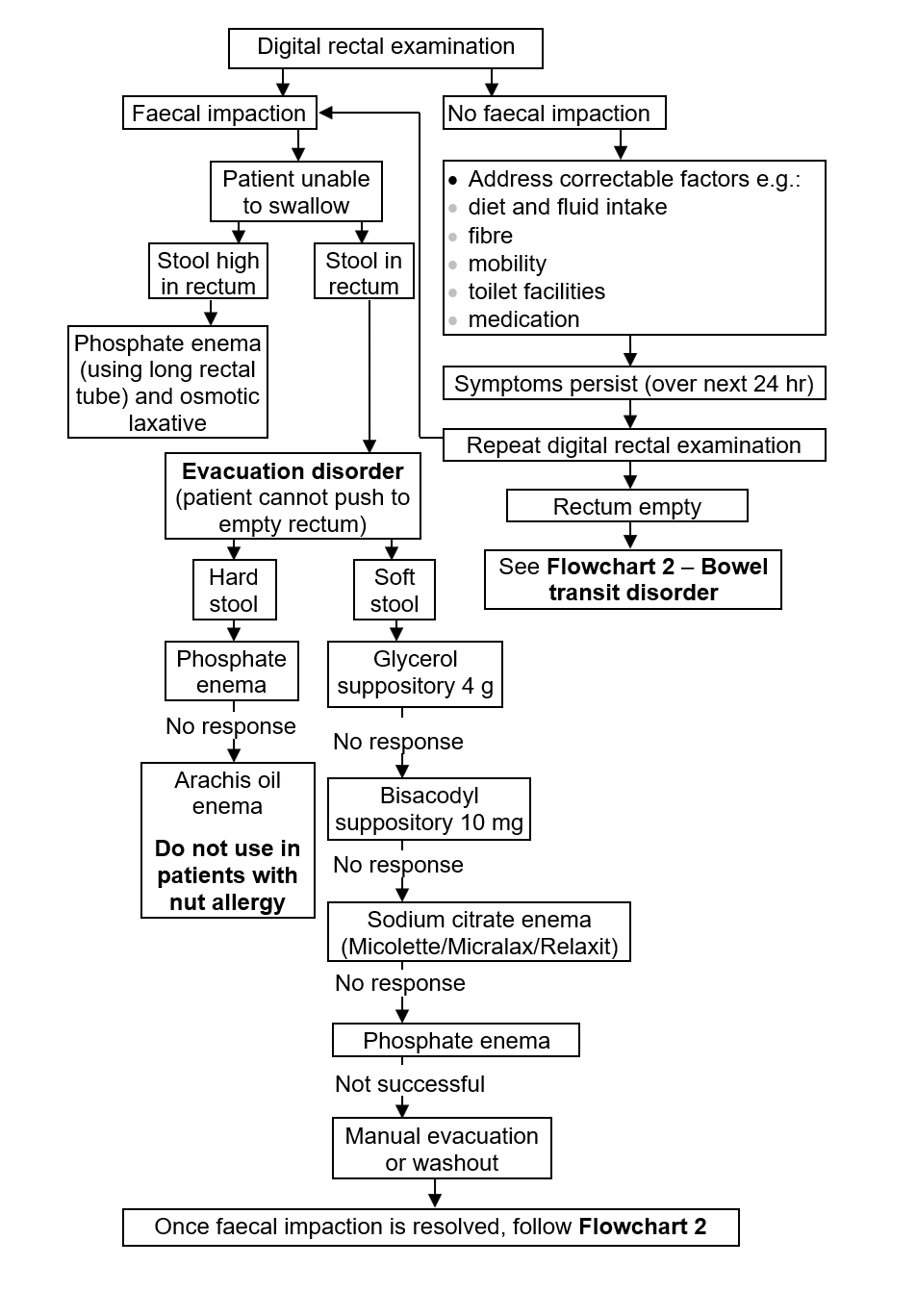
Faecal impaction
Able to swallow
- Use oral route
- Macrogols 4 sachets on first day, then
- increase in steps of 2 sachets daily
- maximum of 8 sachets daily
- total daily dose to be drunk in a 6-hr period
- in patients with moderate to severe heart failure 2 sachets maximum in any 1 hr
- dissolve each sachet in 125 mL water
- use for 3 days maximum
- If faecal impaction is resolved, follow Bowel transit disorder below
- If faecal impaction is not resolved, consider Extra treatment section below
Unable to swallow
- Follow decision algorithm below
Flowchart 1
Bowel transit disorder
- Patient constipated but rectum empty
- Address correctable factors e.g.:
- diet and fluid intake
- fibre
- mobility
- toilet facilities
- medication
Unable to swallow
- If unable to swallow, discuss with consultant
- if patient is very distressed by constipation, consider trial of sodium citrate enema or macrogol given via nasogastric tube
Able to swallow
- Follow Flowchart 2: Bowel transit disorder below
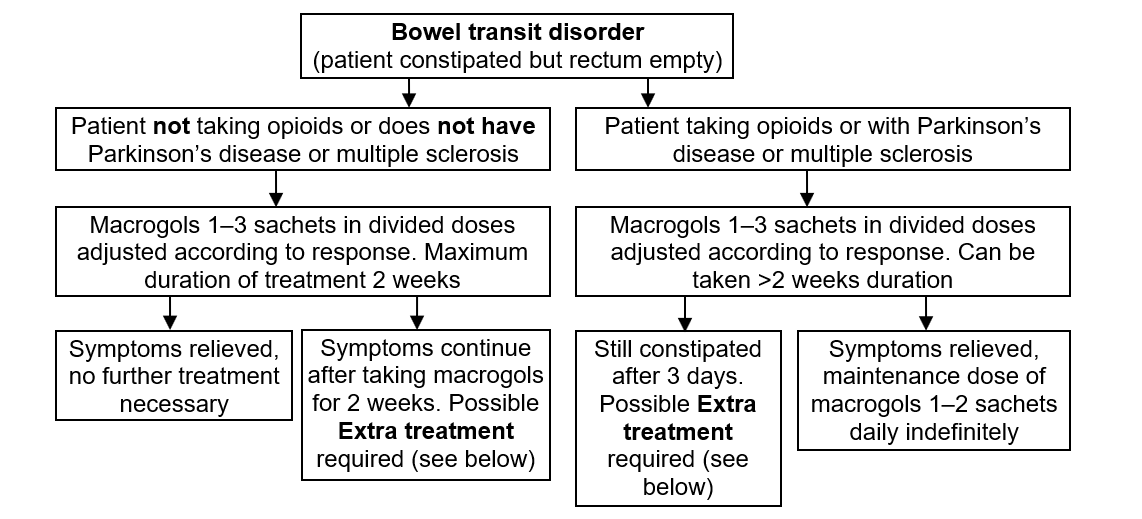
Flowchart 2 – Bowel transit disorder
Extra treatment
- Prescribe other laxatives singly or, if no response, in pairs e.g.:
- ispaghula husk sachet, 1 twice daily, preferably at 0600 hr and 1800 hr or
- senna 2 tablets at night (maximum dose 4 daily), or
- bisacodyl 5-10 mg at night, or
- lactulose 15 mL 12-hrly (this may take up to 24-48 hr to take effect) avoid using 2 osmotic laxatives, macrogol and lactulose at same time; also avoid using senna and bisacodyl at the same time, or
- docusate sodium 100 mg (up to 500 mg daily in divided doses)
- For patients with severe opioid-induced constipation, consider naloxegol 25 mg daily orally
- only prescribe on advice from the palliative care team
Symptoms relieved
- If patient taking opioids, or with Parkinson's disease or multiple sclerosis, continue maintenance dose of the effective treatment daily indefinitely
- If patient not taking opioids, neither has Parkinson’s disease nor multiple sclerosis, further treatment is individual to each patient
Symptoms not relieved
- If patient does not respond to the above medications or 2 of them in combination, consider macrogols again
Last reviewed: 2024-04-24