DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
INDICATIONS
Diagnosis
- Aspirate an acute hot joint of uncertain origin before starting any antimicrobials
- Often used in diagnosis of chronic and subacute articular pathologies
Treatment
- Recurrent aspiration in management of septic arthritis
- Aspiration of tense effusions of any cause
- Before therapeutic intra-articular corticosteroid injection
CONTRAINDICATIONS
- No absolute contraindications to joint aspiration
- Caution in patient with clotting disorder/taking anticoagulants. Discuss with consultant
- Caution in patient with prosthetic joint. Discuss with orthopaedic surgeon
- Avoid passing needle into joint through skin lesion (e.g. psoriasis), as this can lead to joint sepsis
EQUIPMENT
- Sterile dressing pack
- Gloves
- Skin antiseptic
- 20, 10 and 2 mL syringes, green and orange needles
- Lidocaine 1% plain
SPECIMEN BOTTLES
- Blood culture bottles for aerobic and anaerobic culture of synovial fluid
- 2 plain sterile universal containers:
- 1 for Gram staining
- 1 for crystals
- Heparin tube - for white cell count (orange top)
PROCEDURE
- If not competent in procedure, organise supervision by a clinician experienced in the procedure
Consent
- Explain procedure and reassure patient
- Obtain and record consent
Position of patient and site of insertion
- Ask patient to lie supine
- Make sure muscles around joint are relaxed to minimise any discomfort from procedure
- putting pillow under knee may help to relax it
- Identify margins of knee joint and patella
- Mark a point (e.g. with thumbnail) 1 cm below mid-point of medial aspect of patella
Aseptic technique and premedication
- Wash your hands, don gloves, prepare skin around knee
- Infiltrate skin with lidocaine 1% using an orange needle
Sampling
- Use no-touch technique
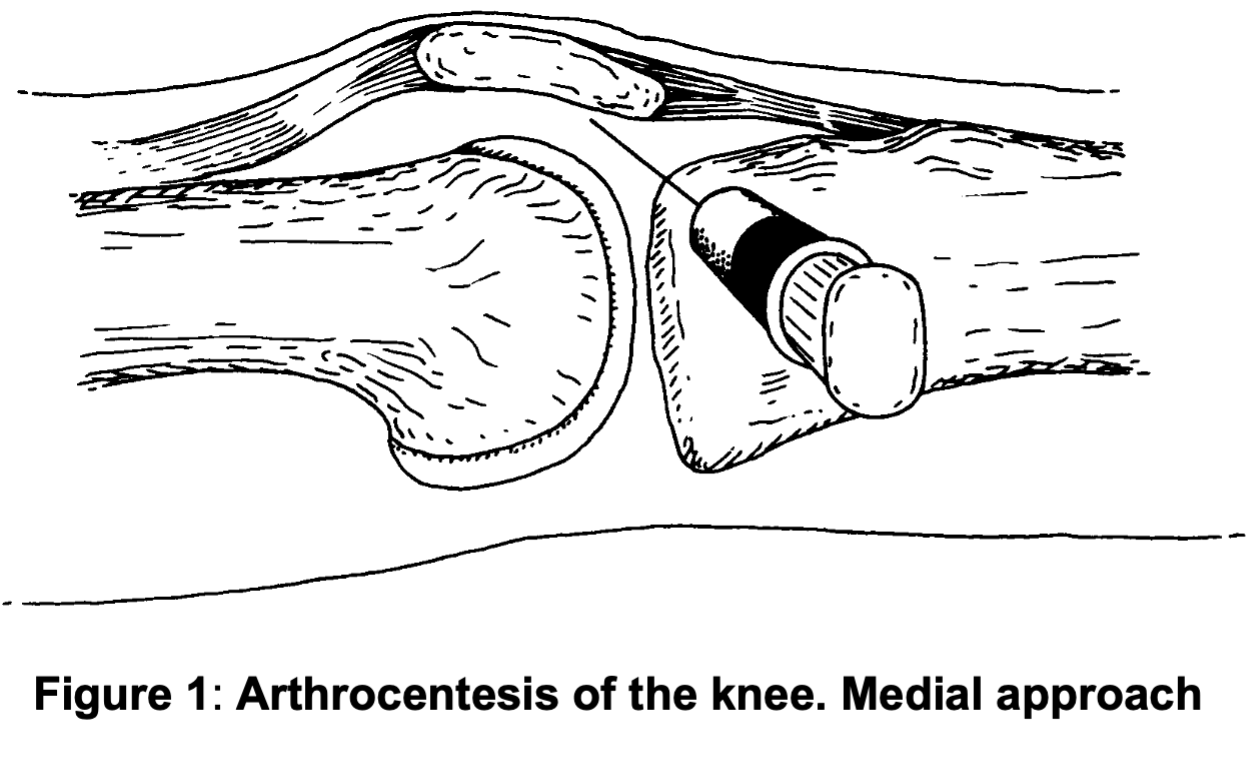
- Insert green needle with 10 or 20 mL syringe horizontally at previously marked point into gap between patella and femur and slightly upward towards suprapatellar pouch
- see figure 1
- if there is only a small effusion, it can help to displace patella medially to increase gap between patella and femur (Figure 1)
- Aspirate while advancing needle and stop advancing if synovial fluid aspirated
- once fluid begins to appear, it can be 'milked down' by pressure with one hand over suprapatellar pouch
- Once syringe full, detach from needle, leaving needle in joint
- Empty syringe into specimen bottles
- 8-10 mL of fluid directly into aerobic bottle first, followed 8-10 mL into anaerobic bottle, rest into plain sterile universal container
- Re-attach syringe to needle and re-aspirate
- Aspirate joint to dryness
- When aspiration complete, withdraw needle
- An adhesive plaster or Micropore dressing to skin is sufficient
Documentation
- Record procedure in notes
- Document exact joint aspirated with:
- volume of fluid
- macroscopic appearance ('frank pus', 'turbid straw-coloured fluid', 'frank blood', 'blood-stained synovial fluid', etc.)
- viscosity ('viscous' or 'thin') of fluid
SPECIMENS
- Send synovial fluid in blood culture bottle and one plain sterile universal container to microbiology
- request urgent Gram stain
Last reviewed: 2023-11-16