DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
If patient NOT NOT PREGNANT, contact obstetric team
DEFINITION
Deep vein thrombosis (DVT) is the development of a thrombus (blood clot) that completely or partially occludes a deep vein, usually in the legs
RECOGNITION
Symptoms and signs
- Swelling of limb (arm, calf or leg)
- measure circumference 10 cm below tibial tuberosity and compare with asymptomatic limb
- difference of >3 cm increases probability of DVT
- Pain and stiffness of affected limb
- Pitting oedema
- Increased skin temperature
- Erythema
- Tenderness
- Mild fever
Pregnancy
- It can be difficult to distinguish symptoms and signs of DVT from normal pregnancy
- exercise vigilance in pregnant woman – discuss with obstetric registrar/specialist trainee
Complications
- In rare cases, arterial circulation may be severely compromised:
- severe pain, swelling, cyanosis
- rapid development of tense blue oedema (phlegmasia cerulea dolens)
- If patient is an injection drug user, examine for:
- localised infection e.g. erythema or fluctuance suggesting infected clot
- deep soft tissue infection, abscess at injection site
- necrotising fasciitis
- acute arterial occlusion, and/or myositis
- systemic infection and septic embolic abscesses e.g. cardiac murmurs suggesting infective endocarditis, sepsis, haemoptysis and cough with purulent sputum
Differential diagnosis
- Ruptured Baker’s cyst
- history of arthritis or trauma to knee
- swelling behind knee
- examine for arthropathy and effusion
- Torn calf muscles/damage to Achilles tendon
- sudden pain in calf following twisting of leg
- examine for haematoma
- disruption of tendon indicates severe rupture
- Cellulitis – see Cellulitis guideline
- Fracture
- Oedema (heart failure, hypoalbuminemia, lymphatic obstruction, dependant)
- Acute Charcot arthropathy
- consider if longstanding diabetic with peripheral neuropathy and/or history of trauma
- advise reducing weight bearing
- refer urgently to diabetic nurse, podiatry and orthopaedics
INVESTIGATIONS
- FBC, INR, APTT, LFTs, and U&E
- If patient is an injection drug user or has signs of infection:
- CRP
- blood cultures
- chest X-ray (to exclude septic embolic lung abscesses)
- ultrasound of groin area (localised collection)
- echo if murmur, positive blood cultures or chest X-ray suggestive of septic embolic lung abscesses
- offer testing for blood borne viruses (HIV, HBV, HCV) – see HIV infection testing guideline
D-dimer
- Raised in many clinical states. See Common causes of raised D-dimer concentration
- normal D-dimer concentration virtually rules out thrombosis
Common causes of raised D-dimer concentration
- Acute myocardial infarction (MI)
- Chronic subdural haematoma
- Disseminated intravascular coagulation
- Gram-negative bacteraemia
- Leukaemia
- Liver disease
- Metastatic malignancy
- Peripheral vascular disease
- Pregnancy
- Recent surgery
- Renal disease
- Rheumatoid disease
- Sickle cell crisis
- Subarachnoid haemorrhage
- Thrombolytic therapy
- Trauma with pathological thrombosis
ASSESSMENT
- If DVT suspected in a woman who is pregnant or has given birth within the last 6 weeks:
- Do not use two-level DVT Wells score
- immediately commence dalteparin. See Dalteparin for VTE guideline
- refer immediately for same-day Doppler scan
- discuss with obstetrics registrar/specialist trainee
Doppler scan negative
- If low clinical suspicion of DVT, discontinue treatment
- If DVT clinically likely, continue treatment and repeat Doppler scan in 6–8 days
- if positive, continue treatment
- if negative, discuss other imaging modalities with radiologist and obstetric consultant
Doppler scan positive
- Discuss with obstetric registrar or specialist trainee
- Commence/continue treatment for DVT
Calculate two-level DVT Wells score using tool
Table 1: Two-level DVT Wells score
| Clinical feature | Points |
| Paralysis, paresis or recent plaster immobilisation of lower extremities | 1 |
| Recently bedridden for ≥3 days or major surgery within 12 weeks requiring general or regional anaesthesia | 1 |
| Localised tenderness along distribution of deep venous system | 1 |
| Entire leg swollen | 1 |
| Calf swelling at least 3 cm larger than asymptomatic side. Measure circumference 10 cm below tibial tuberosity | 1 |
| Pitting oedema confined to symptomatic leg | 1 |
| Malignancy (on treatment, treated in last 6 months or palliative) | 1 |
| Collateral superficial veins (non-varicose) | 1 |
| Previously documented DVT | 1 |
| An alternative diagnosis is at least as likely as DVT | -2 |
| Clinical probability simplified score | |
| DVT likely | ≥2 points |
| DVT unlikely | ≤1 point |
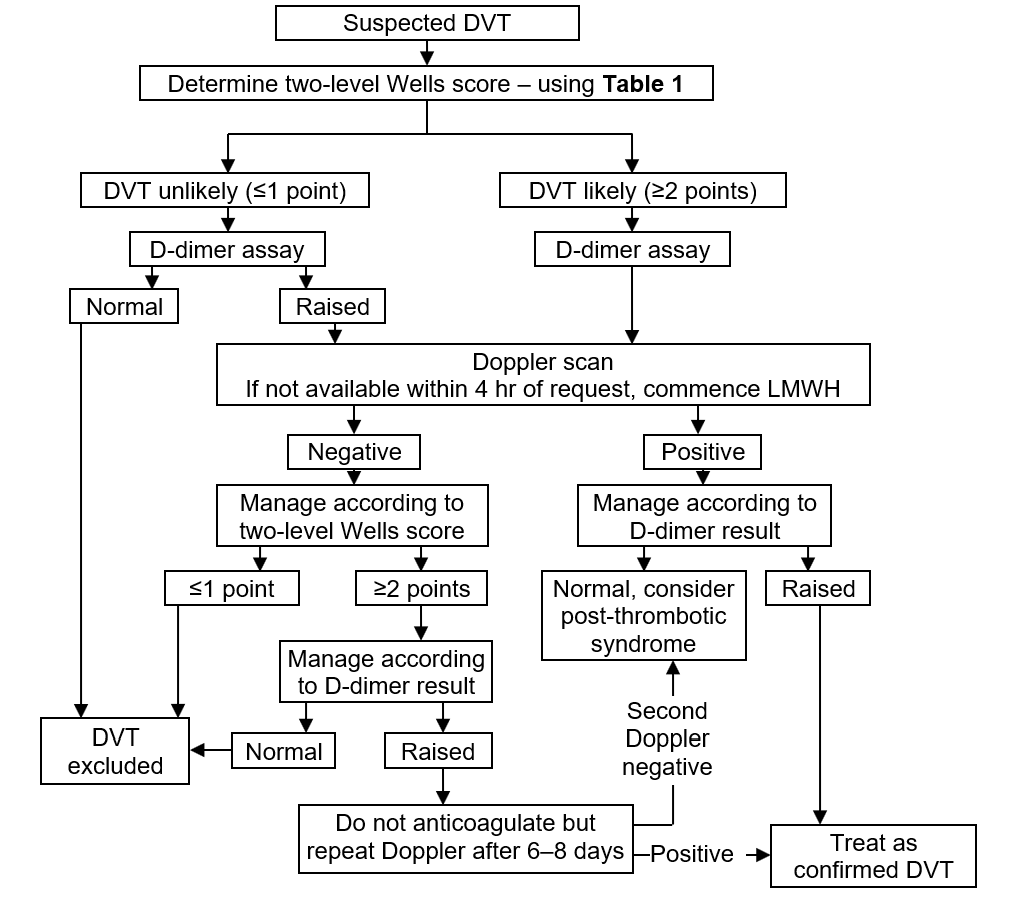
Flowchart for DVT management
D-dimer result available
- Select calculated two-level DVT Wells Score and D-dimer combination
Doppler scan indicated
- Local booking instructions
- If Doppler ultrasound scan cannot be arranged within 4 hr of request, but patient can otherwise be discharged:
- start SC dalteparin (see Dalteparin for VTE guideline) or direct oral anticoagulants (see DOAC in VTE guideline)
- if delay >24 hr (e.g. bank holiday), follow local instructions
Doppler and D-dimer results available
Select correct Doppler result, DVT Wells Score and D-dimer combination - see Flowchart for DVT management
MANAGEMENT
- Encourage ambulation
- Elevation of leg when seated
- Simple analgesia (e.g. paracetamol or if inadequate control, co-codamol)
- Discuss with obstetric registrar/specialist trainee
- Dalteparin and warfarin are not contraindicated in breastfeeding
- Either continue dalteparin (see Dalteparin for VTE guideline) for 8–12 weeks followed by prophylactic dose for the rest of pregnancy and ≥6 weeks postnatally. See Prophylaxis against venous thromboembolism guideline
- Or if woman chooses to commence warfarin to complete anticoagulation treatment postpartum, avoid until third postnatal day. See Warfarin initiation guideline
- If anticoagulation contraindicated, consultant physician, staff physician must decide which carries most risk – complications of therapy (consider vena caval filter) or DVT/PE
Inferior vena caval filter (IVCF)
- IVC filters carry significant morbidity and mortality risks and only be offered if:
- anticoagulation treatment contraindicated in confirmed proximal DVT or PE. Remove IVCF when anticoagulation treatment
- no longer contraindicated and has been established
- person with proximal DVT or PE has a PE while taking anticoagulation
- Discuss with haematologist before requesting IVCF treatment only
- Before fitting an IVCF, ensure there is a strategy in place and documented for removal at earliest possible opportunity
Choice of anticoagulation long-term
Warfarin preferred if:
- History of antiphospholipid syndrome
- Interacting medication
- Concurrent metallic heart valve
- Recurrent thrombosis whilst therapeutically anticoagulated
LMWH therapy for duration of treatment preferred if:
- Injection drug user
- Active cancer, particularly luminal GI and GU neoplasms
- At risk of GI bleeding
- If continuing with dalteparin, inform local anticoagulation service
Start of anticoagulation
- Start as soon as PE suspected
- If aiming to continue anticoagulation long-term with dalteparin, warfarin, edoxaban or dabigatran, commence dalteparin - see Dalteparin for VTE and DOAC for VTE guidelines
- If aiming to continue anticoagulation long-term with apixaban or rivaroxaban, start DOAC immediately - see DOAC for VTE guideline
DVT confirmed
- Start chosen long-term anticoagulant
- if continuing anticoagulation with warfarin, edoxaban or dabigatran, continue dalteparin (see Dalteparin for VTE guideline) for minimum of 5 days
- For details of drugs see DOAC in VTE guideline or Warfarin initiation guideline
COMPLICATIONS
Suspected phlegmasia cerulea dolens (painful blue oedema)
- An uncommon manifestation of massive DVT compromising venous outflow and causing ischemia and manifesting as a painfully swollen blue leg
- Elevate bed foot to 40° and ensure fluid replacement adequate to compensate for extravasation
- Refer urgently to on-call general surgical team
Concomitant infection
- Treat cellulitis or sepsis – see Cellulitis guideline and Sepsis guideline
- If evidence of groin abscess, refer to on-call surgical team
- If evidence of septic pulmonary embolism on chest X-ray, admit to respiratory or infectious diseases ward
Symptomatic ileo-femoral DVT
- Suggested by back pain and swelling of entire limb
- Discuss with radiologist (and if pregnant, obstetrician) to consider magnetic resonance venography
Treatment
- Consider catheter guided thrombolysis or mechanical thrombectomy if:
- symptoms of <14 days duration
- good functional status
- life expectancy of ≥1 yr
- low risk of bleeding (for thrombolysis)
- Discuss with interventional radiologist and vascular surgeon
- Do not prescribe elastic graduated compression stockings to prevent post-thrombotic syndrome or VTE recurrence after a proximal DVT
SCREENING
- If no clear precipitating cause for thrombosis, particularly if this is a recurrent event, consider occult malignancy or other cause of thrombophilia
- If patient aged <45 yr with unprovoked DVT, discuss screening for inherited or acquired thrombophilia with haematology consultant
Screen for cancer
- In all patients with confirmed DVT, chest X-ray, FBC, LFT, calcium and urinalysis
- Only offer further investigations for cancer to people with unprovoked DVT if they have relevant symptoms or signs
DISCHARGE
Outpatient
- Unless symptoms severe, or patient an injection drug user, or requires admission to hospital for reasons other than suspected DVT, treat as outpatient
- ensure form authorising daily injections of dalteparin completed once diagnosis confirmed
Duration of treatment
- Treatment will be continued for 3 months, but duration may be longer if DVT was unprovoked, recurrent or in the presence of cancer or non-modifiable risk factor such as significant immobility
Advice to patient
- Many drugs (including alcohol) interact with warfarin or DOAC
- To remind their GP, if additional medication is added, that they are taking anticoagulant
- To inform dentist that they are anticoagulated
- Give advice on extended travel
- Provide PE information booklet
Women of childbearing age (Pregnancy, Pills, Periods)
- Counsel that DOACs and warfarin may be harmful in pregnancy.
- seek immediate advice if pregnant or trying to conceive
- Anticoagulation may lead to menorrhagia in 70% of women. Apixaban less commonly implicated than warfarin and rivaroxaban
- Do not stop contraception at time of PE diagnosis including combined oral contraceptive pill (COCP)
- Refer patient to thrombosis clinic to discuss options
- Anticoagulation negates the ongoing thrombotic risk of the COCP. Stopping COCP may precipitate menorrhagia or lead to pregnancy whilst on a DOAC
Monitoring of warfarin
- Refer to anticoagulant management service for follow-up appointment date
- Give patient a completed yellow anticoagulation therapy record - see Warfarin for VTE guideline
- Ensure discharge letter includes diagnosis, dosage of warfarin and date of clinic appointment
- If anticoagulation to be monitored by GP, supply GP with written information (on separate sheet, stapled to discharge letter) about:
- indication for anticoagulation
- proposed duration of treatment
- proposed target range for INR
- details of anticoagulation in hospital (give dates, INR results and dosage taken)
Document
- Document in medical record
- patient has been given written and verbal information about warfarin and has been referred to anticoagulation clinic
- duration of treatment
- if definite risk factor identified
- outpatient investigations
- monitoring arrangements
Follow-up
- Arrange appointment in 10-12 weeks for appropriate medical clinic
- unless a shorter course of treatment or need for investigation requires earlier follow-up; patients with confirmed DVT remain under the care of duty physician for the day on which diagnosis was confirmed
- send copy of letter to patient’s GP
FOLLOW-UP CLINIC
- If patient has active cancer, reassess risks and benefits of continuing anticoagulation at 6 months
- After a first proximal DVT without a clear underlying cause or if permanent risk factors present, assess VTE risk and discuss with patient, if anticoagulation should be continued
Last reviewed: 2025-07-10