DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
RECOGNITION AND ASSESSMENT
Symptoms and signs
- Often none, or neuromuscular symptoms (e.g. muscle weakness, absent reflexes, ileus)
Investigations
Immediate
- ECG changes - depressed ST, flat T, U waves, arrhythmias (arrhythmias may cause cardiorespiratory symptoms)
Helpful
- Take sample from arm without a drip
- Venous HCO3- - when raised (metabolic alkalosis) indicates chronic depletion; if <22 mmol/L in absence of GI loss, suspect renal tubular acidosis - refer to renal team
- Urine K+ if cause not obvious
- Serum magnesium (Mg2+) for persistent urine K+ loss especially patients with diarrhoea or on diuretics
Common Causes
- Blood taken from drip arm (artefact)
- Any excessive gastrointestinal fluid loss
- Renal loss: urine K+ >20 mmol/L - diuretics, mineralocorticoid excess (hyperaldosteronism and excess cortisol), Mg2+ deficiency see Hypomagnesaemia guideline, and renal tubular disease
- Intracellular shift (redistribution): insulin or bicarbonate treatment, theophylline, beta2 agonists, periodic paralysis, rapid blood cell proliferation
- Intravenous fluid therapy, with inadequate electrolyte replacement
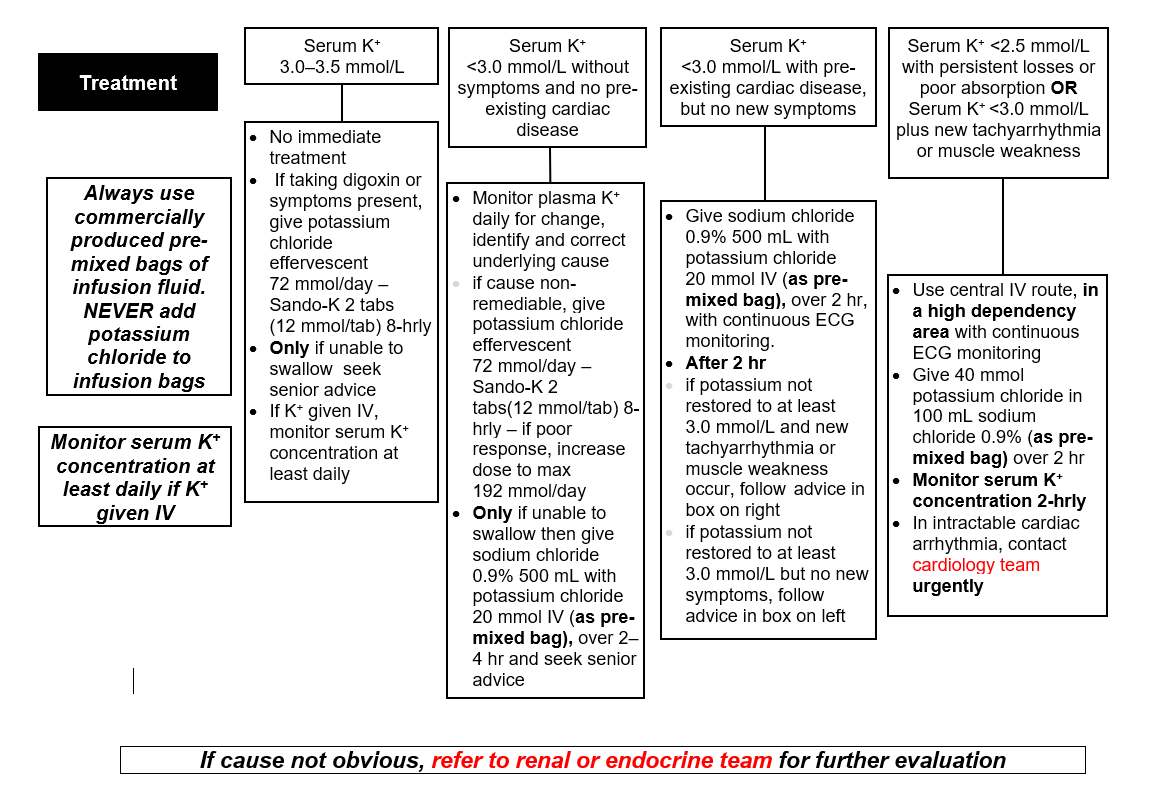
MANAGEMENT
Always use commercially produced pre-mixed bags of infusion fluid. NEVER add potassium chloride to infusion bags
- Manage K+. For guidance follow tool below
- Treat the underlying cause. If cause not obvious, refer to renal or endocrine team for further evaluation
Last reviewed: 2024-03-06