DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
SPECIFIC CONDITIONS
If patient has any of the following conditions, follow appropriate condition-specific guideline
- For neutropenic sepsis in cancer patients – see Neutropenic sepsis guideline
- For sepsis management in children – see Paediatric guidelines
- For peri-natal sepsis – see Obstetric and Neonatal guidelines
DEFINITIONS
- Sepsis – a life-threatening organ dysfunction due to dysregulated host response caused by an infection. It is a medical emergency
- Septic shock is associated with a higher risk of mortality (>40%) and refers to patients with sepsis who:
- remain hypotensive despite adequate fluid resuscitation and require vasopressors to maintain a mean arterial pressure (MAP) ≥65 mmHg
- have persistently elevated serum lactate (≥2 mmol/L)
SCREENING
- All patients who have a NEWS ≥5 (or) any individual NEWS element ≥3, screen for sepsis by completing Sepsis Proforma Looking for red flags and moderate risk factors
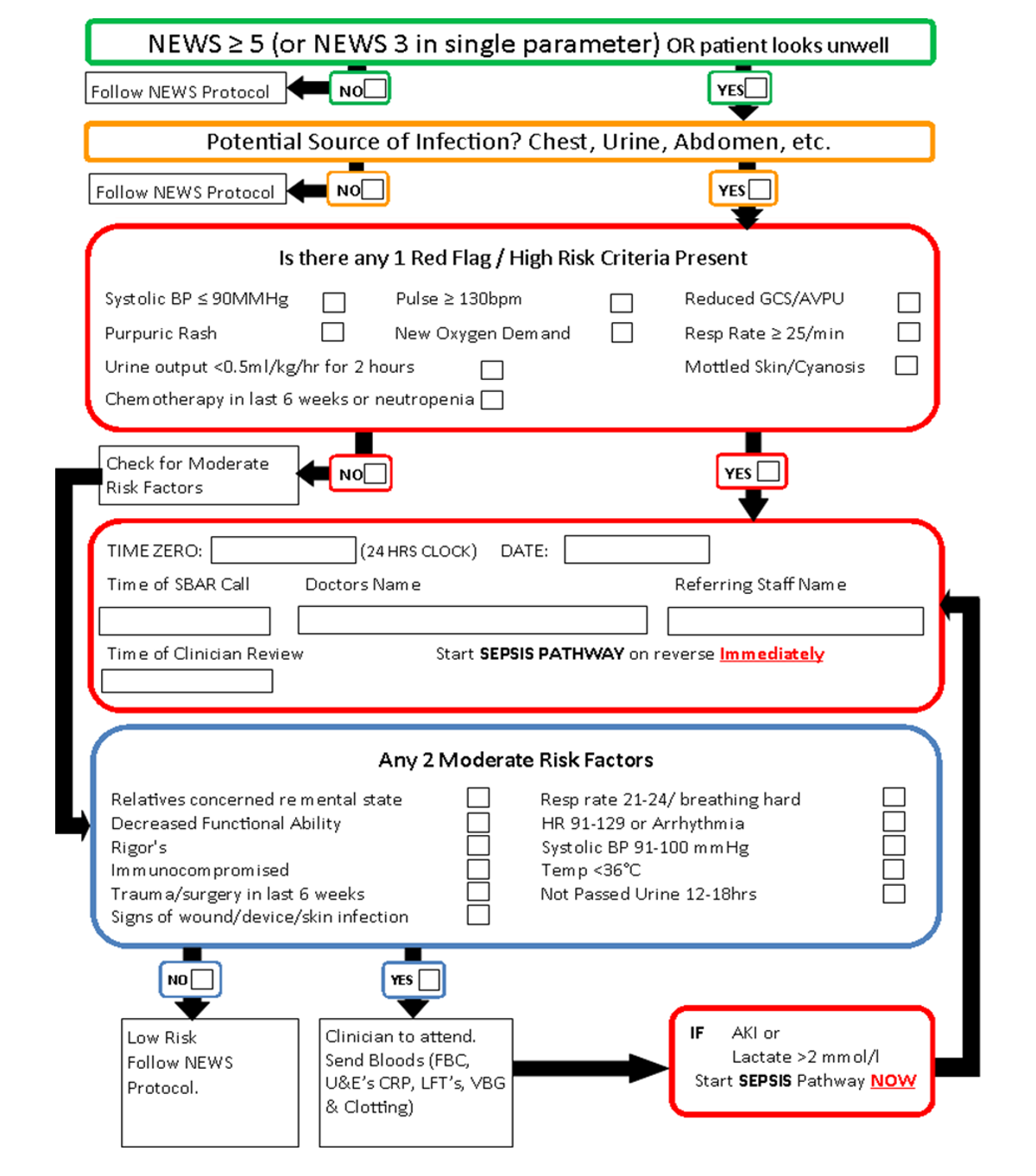
IMMEDIATE MANAGEMENT
- Start Sepsis Six if the patient satisfies 1 of the following:
- presence of 1 red flag sign or
- presence of 2 moderate risk factors along with AKI and/or lactate ≥2
Sepsis Six
- Complete all actions in one hour
- Ensure senior clinician attends
- Administer Oxygen
- Obtain IV access
- Take blood cultures, glucose, lactate, FBC, U&Es, CRP and clotting
- Consider cultures from potential sources of infection & Chest X-ray
- if probable CNS infection, perform lumbar puncture. See Lumbar puncture
- Give IV antimicrobials
- Give IV fluids
- see Adult fluid management guideline
Monitor
- NEWS2. See NEWS
- Measure urine output
- may require urinary catheter
- start fluid balance chart & complete hrly
- Check serial lactates
- corroborate high VBG lactate with arterial sample
- If lactate >4mmol/L, call critical care
- Record observations at least every hour
- if initial lactate raised or if clinical condition deteriorates, at least every 30 minutes
Antimicrobials
Penicillin Allergy
- True penicillin allergy is rare
- Ask the patient and record what happened when they were given penicillin
- If any doubt about whether patient is truly allergic to penicillin, seek advice from a microbiologist or consultant in infectious diseases
Only accept penicillin allergy as genuine hypersensitivity if convincing history of either rash within 72 hr of dose or anaphylactic reaction
Infection Control alerts
- Check for IC alert
- if IC alert not available, check previous 12 months of microbiology reports
- If MRSA present, treat as tagged for MRSA. See MRSA management
- high risk of MRSA: recent history of MRSA, patient in other hospital/nursing home in last 12 months, sepsis likely to be hospital-acquired, or line infection suspected
- If ESBL, MGNB, CARB present, treat as tagged for ESBL. See ESBL/MGNB/CARB management
- ESBL or MGNB tag: history of ESBL-producing or multi-resistant Gram-negative Bacilli
Choice of anti-microbials
Select type of patient from list:
- First line: Meropenem 0.5-1 g IV 8-hrly plus vancomycin IV by infusion – see Vancomycin guideline
- Alternative (true penicillin allergy): Meropenem 0.5-1 g IV 8-hrly plus vancomycin IV by infusion – see Vancomycin guideline. If anaphylaxis to penicillin, discuss with consultant in infectious diseases or microbiologist
- First line: Piperacillin/tazobactam 4.5g IV infusion 8-hrly plus vancomycin IV by infusion – see Vancomycin guideline
- Alternative (true penicillin allergy): Aztreonam 2g IV 6-8-hrly plus vancomycin IV by infusion – see Vancomycin guideline
- First line: Meropenem 0.5-1g IV 8-hrly alone
- Alternative (true penicillin allergy): Meropenem 0.5–1 g IV 8-hrly alone. If anaphylaxis to penicillin, discuss with consultant in infectious diseases or microbiologist
- First line: Piperacillin/tazobactam 4.5 g IV infusion 8-hrly (if necessary, increase to 4.5g IV 6-hrly; increased frequency may be used for severe infections)
- Alternative (true penicillin allergy): Aztreonam 2g IV 6-8-hrly plus vancomycin IV by infusion - see Vancomycin guideline
Septic shock
- Consider patient in septic shock if any of the following are present despite 30 mL/kg of fluid resuscitation within first 3 hr
- mean arterial blood pressure ≤65 mmHg or
- serum lactate persistently elevated ≥2 mmol/L on repeated measurements
- Consider immediate escalation to senior clinician (registrar and above) and/or to critical care team
- Once decision is made, admit patients requiring critical care to the ICU within 6 hours
CODING FOR DIAGNOSIS OF SEPSIS
- Correct coding of sepsis enables local and national data to accurately reflect the incidence of sepsis
- Current consensus definition is 'organ dysfunction' and dysregulated host response secondary to an infectious source
- Do not document localised infections (non-septic infections) in medical record as sepsis (e.g. terms like urosepsis, biliary sepsis, chest sepsis etc., may be inaccurately coded as systemic sepsis)
- good practice is for a responsible consultant to confirm that initial diagnosis of sepsis is a 'true sepsis' or indicate only a localised infection present (rather than generalised sepsis), code as a localised infection only or a 'non-septic infection'
Last reviewed: 2023-10-23