DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
RECOGNITION AND ASSESSMENT
- Anaphylaxis is a severe systemic allergic reaction
- Consider if rapid onset of respiratory difficulty and/or hypotension
- especially if rash and/or angioedema present
Symptoms and signs
Airway
- Upper airways obstruction due to angioedema:
- swelling of tongue/throat
- stridor
- feeling of throat closing
- hoarse voice
Breathing
- Lower airways obstruction:
- wheeze
- increased respiratory rate
- cyanosis
Circulation
- Signs of shock:
- impaired capillary refill (capillary refill time >2 sec)
- tachycardia
- hypotension
Disability
- Confusion
- Agitation
- Loss of consciousness
Exposure
- Skin and mucosal changes (may not be present in all patients):
- redness or blotchy rash
- urticaria
- itching
- angioedema
- rhinitis and conjunctivitis
Other systems affected
- Gastrointestinal:
- abdominal pain
- vomiting
- diarrhoea
Investigations
- Mast cell tryptase - sample serum at following times
- take first sample as soon it can be taken without delaying treatment
- second sample at 1-2 hr from onset of symptoms. No later than 4 hr
- Patient may present late. Take as many serum samples as time since presentation allows
- indicate time and date clearly to allow interpretation of results
- Inform patient that a final sample at least 24 hours after complete resolution will be necessary to measure baseline levels in follow-up
Differential diagnosis
- Syncope (rapid recovery) with bradycardia in vagal reaction
- Septic shock with a petechial or purpuric rash
- Acute cardiac event
- Panic attack with hyperventilation (unlikely to be hypotensive)
- Acute severe asthma
- Other causes of central airways obstruction
- inducible laryngeal obstruction (previously called vocal cord dysfunction)
- ACE inhibitor-induced laryngeal angioedema
- Idiopathic non-allergic urticaria and angioedema
IMMEDIATE MANAGEMENT
- All doses are for adults
Diagnosis
Look for
- Acute onset of illness
- Life-threatening Airway and/or Breathing, and/or Circulation problems
- Airway: Swelling, hoarseness, stridor
- Breathing: Rapid breathing, wheeze, fatigue, cyanosis, SpO2 <92%, confusion
- Circulation: Blotchy and red, clammy, low blood pressure, faintness, drowsy/coma
- Usually skin changes
- Recent exposure to an allergen known to affect them
Call for help
- Lay patient flat and elevate feet to restore/maintain BP. Do not stand patient up
- if pregnant, lie on left side
- if this causes respiratory distress, sit patient up
IM Adrenaline
- For hypotension or respiratory distress with stridor or wheezing, give adrenaline:
- 500 microgram (0.5 mL of 1:1000 solution) IM into midpoint of anterolateral aspect of thigh
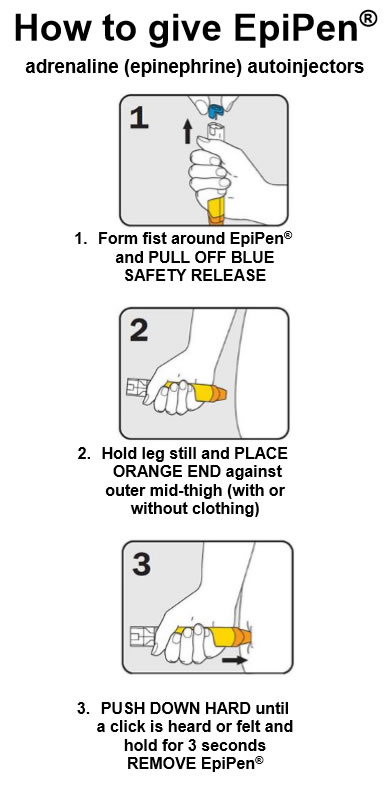
- if an adult EpiPen® is more readily available give this (delivers 300 microgram dose of adrenaline)
- If hypotension and respiratory distress do not respond within 5 min:
- give further dose of adrenaline 500 microgram IM (0.5 mL of 1:1000 solution)
- Can be repeated at 5 min intervals according to BP, heart rate and respiratory function
- monitor vital signs continuously
IV adrenaline is hazardous
- Use only with extreme care, and under critical care supervision. Seek expert help for use of IV adrenaline early
- for those in profound shock that is immediately life-threatening
- for those whose respiratory and/or cardiovascular problems persist despite 2 doses of IM adrenaline. See Refractory anaphylaxis below
When skills and equipment available
Establish airway
- If concerned about patient's respiratory effort/airway obstruction, contact anaesthetist
High-flow oxygen
- Oxygen at high flow rate (10-15 L/min) - see Oxygen therapy in acutely hypoxaemic patient guideline
IV fluid challenge
- Establish IV access
- If systolic BP <100 mmHg, give fluid challenge of compound sodium lactate (Hartmann's) 500-1000mL as quickly as possible. See Fluid resuscitation guideline
- Stop IV colloid if this might be cause of anaphylaxis
Bronchospasm
- If there is bronchospasm, give salbutamol 5 mg via oxygen driven nebuliser
- for further treatment of bronchospasm, see Asthma guideline
REFRACTORY ANAPHYLAXIS
- If no response to 2 doses of IM adrenaline:
- continue to give further doses of IM adrenaline every 5 minutes until infusion established
- contact critical care team to set up IV adrenaline infusion
- rapid IV fluid infusion. A large volume (up to 3 - 5 litres in adults) may be needed for severe anaphylactic shock
- Patients taking regular beta-blockers may be refractory to adrenaline. Consider using glucagon if no response to adrenaline and IV fluids. Monitor for adverse events, including hyperglycaemia, vomiting, hypokalaemia and hypocalcaemia
Further treatment under critical care supervision
- Consider giving adrenaline 50 microgram (0.5 mL of the ready dilute 1:10,000 adrenaline injection) by slow IV injection, no faster than 1 mL/min while monitoring cardiac rhythm
- repeat according to response
- If multiple doses required, give adrenaline as slow IV infusion, stopping when response obtained
MONITORING
- Monitor (including ECG) continuously all patients experiencing severe anaphylaxis until condition stabilised
- then every 15 min for 1 hr until completely stable
- Continue to record hourly:
- heart rate
- blood pressure
- respiratory rate
- if possible, peak expiratory flow (PEF)
- SpO2
SUBSEQUENT MANAGEMENT
- Record time of onset of symptoms and identify possible allergens
- e.g. drugs, foods (within previous hour), insect stings, latex
- Observe until all allergic symptoms have subsided completely, consider prednisolone 30 mg oral daily
Rash
- Cetirizine 10mg oral daily for management of rash
- If the oral route is not possible, chlorphenamine 10mg by IM or slow IV injection
Observation
- Warn patient of possible early recurrence
≥12 hr observation
Any of:
- Severe reaction requiring >2 doses of adrenaline
- Patient has severe asthma or reaction involved severe respiratory compromise
- Possibility of continuing absorption of allergen, e.g. slow-release medicines
- Patient presents late at night, or may not be able to respond to any deterioration
- Patients in areas where access to emergency care is difficult
Minimum 6 hours observation after resolution of symptoms
Any of:
- 2 doses of IM adrenaline needed to treat reaction
- Previous biphasic reaction
2 hours observation after resolution of symptoms
Consider fast track discharge if all of:
- Good response (within 5-10 minutes) to a single dose of adrenaline given within 30 minutes of onset of reaction
- Complete resolution of symptoms
- The patient already has unused adrenaline auto-injectors and has been trained how to use them
- There is adequate supervision following discharge
DISCHARGE AND FOLLOW-UP
- Senior clinician reviews patient before discharge
- Patient given clear instructions to return to hospital if symptoms return
- Advise avoidance of allergen if appropriate
- Management plan to include use of antihistamines for any allergic symptoms and EpiPen® and 999 call for life-threatening symptoms of dyspnoea or faintness
- Prescribe 2 auto-injector devices containing adrenaline 300 microgram (EpiPen®)
- instruct patient on when and how to use
- Give patient contact details for SOS Talisman (0208 554 5579 or www.sostalisman.co.uk) or MedicAlert® (01908 951045 or www.medicalert.org.uk) to obtain alert jewellery containing vital information on their condition in case of emergency
- Give patient contact details of Anaphylaxis Campaign 1 Alexandra Road, Farnborough, Hampshire GU14 6BU (01252 546100) www.anaphylaxis.org.uk
- Send outpatient referral to the allergy clinic
Last reviewed: 2024-04-29