DO NOT USE - ALL INFORMATION LIKELY INCORRECT IF NOT ACTIVELY DANGEROUS
Please use current guidelines available on the UHNM intranet for patient treatment
Please use current guidelines available on the UHNM intranet for patient treatment
RECOGNITION AND ASSESSMENT
- Complete asthma pathway
Symptoms and signs
- Cannot complete sentences in one breath
- Respiration ≥25 breaths/min
- Pulse ≥110 beats/min
- Use of accessory muscles
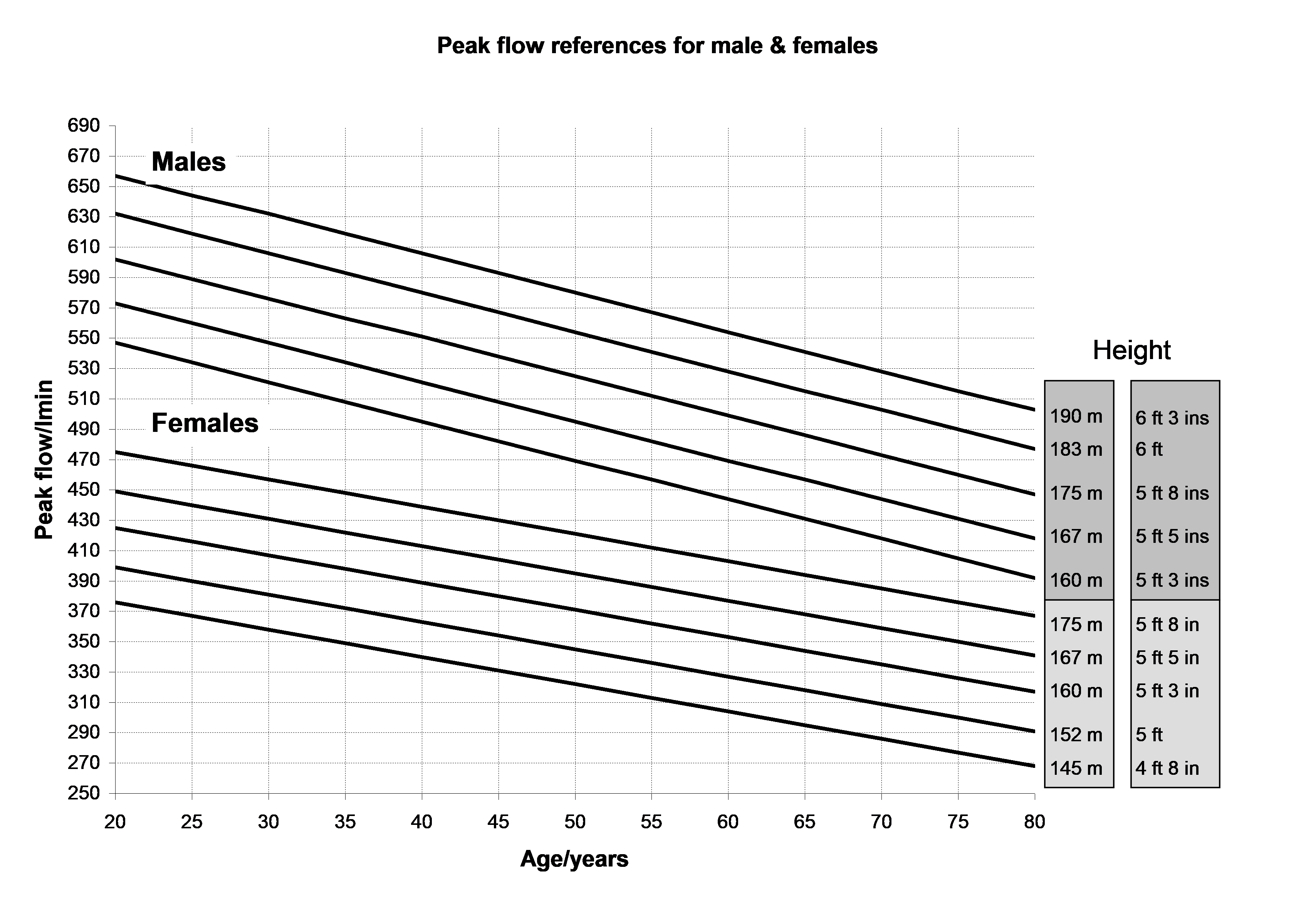
- Peak expiratory flow (PEF) <50% of predicted or best (if known)
Life-threatening features
- PEF <33% of predicted or best (if known)
- SpO2 <92%
- Silent chest, cyanosis, or feeble respiratory effort
- Bradycardia or hypotension
- Exhaustion, confusion or coma
- Patients with severe/life-threatening attacks:
- may not be distressed and
- may not have all these abnormalities
The attack is life-threatening even if only one of these features
Investigations
Only investigations needed before immediate treatment are:
- PEF
- Oximetry
- If SpO2 <92% or patient has any life-threatening features or not responding to treatment, measure arterial blood gases (ABG)
ABG markers of a life-threatening attack
- Normal or high PaCO2 (>4.6 kPa)
- Severe hypoxia: PaO2 <8 kPa irrespective of treatment with oxygen
- Low pH (or high H+)
IMMEDIATE TREATMENT
- Oxygen: follow Hypoxaemia guideline
- CO2 retention not usually aggravated by oxygen therapy in asthma
- Salbutamol 5 mg or terbutaline 10 mg plus ipratropium 500 microgram via oxygen-driven nebuliser 6-8 L/min oxygen
- Either prednisolone tablets 40 mg
- if taking maintenance prednisolone, increase daily dose by 40 mg; maximum 60 mg
- Or hydrocortisone (preferably as sodium succinate) 100 mg slow IV bolus
- Or both if very ill
- No sedatives of any kind
- If symptoms and signs suggest a bacterial infection, prescribe antimicrobials
- Chest physiotherapy not indicated
- Assess and treat hypovolaemia and electrolyte imbalance - see Adult fluid management guideline and Electrolyte disturbances guidelines:
Further investigations
- Chest X-ray
- U&E (use green top bottle for accurate K+ concentration)
- FBC
- If patient taking theophylline/aminophylline, serum theophylline
Patients with life-threatening features
DO NOT LEAVE THE PATIENT
- Ask medical SpR, staff physician or consultant physician, ideally respiratory, to review urgently
- stay with patient
- Give magnesium sulphate 2g made up to 50 mL with sodium chloride 0.9% by IV infusion over 20 min if not already given earlier (e.g. in ambulance)
- ensure cardiac monitoring and oximetry in situ as risk of hypotension
- never give second dose of magnesium sulphate without discussion with consultant respiratory physician
- Speak to critical care unit (CCU) and transfer patient urgently if continues to deteriorate with:
- falling PEF, worsening or persisting hypoxia, or hypercapnia
- exhaustion, feeble respirations, confusion, or drowsiness
- coma or respiratory arrest
- En-route to CCU, ensure patient is accompanied by a doctor (usually an anaesthetist) prepared to intubate if patient’s clinical condition requires it
SUBSEQUENT MANAGEMENT
- Admit to a respiratory ward or acute medical unit
- Lower threshold for admission in patients with:
- history of non-adherence
- lives alone, mental health issues, learning difficulties
- previous near fatal attack/difficult asthma
- presenting at night
- pregnancy
- Correct disturbances in fluid and electrolyte balance, especially potassium (K+)
- always use commercially produced pre-mixed bags of infusion fluid
NEVER add potassium chloride to infusion bags
If patient improving
- Continue oxygen. See Hypoxaemia guideline
- Prednisolone daily at dose in Immediate treatment section
- if unable to tolerate oral medication, hydrocortisone 100 mg 6-hrly as slow IV bolus over 1 min
- Nebulised salbutamol 2.5 mg plus ipratropium 250 microgram 6-hrly
- Continue regular inhaled/oral preventer medication
- Refer to asthma team
- Change to discharge medication 24 hr before discharge
If patient not improving after 15-30 min
- Continue oxygen to maintain SpO2 >94%
- Give nebulised salbutamol 5 mg more frequently, up to every 15-30 min
- Give ipratropium 500 microgram 4-hrly until patient improving
- Once patient improving, reduce nebulised salbutamol to 2.5 mg and ipratropium to 250 microgram 6-hrly
If patient still not improving after 60 mins
- Ask medical senior physician, ideally respiratory, to review urgently
- Give magnesium sulphate 2g made up to 50 mL with sodium chloride 0.9% by IV infusion over 20 min if not already given earlier (e.g. in ambulance)
- ensure cardiac monitoring and oximetry in situ as risk of hypotension
- never give second dose of magnesium sulphate without discussion with consultant respiratory physician
- Senior clinician to consider use of aminophylline or salbutamol by infusion - see Aminophylline guideline and Salbutamol guideline for doses
- if patient already taking oral theophylline DO NOT give loading dose IV aminophylline
- cross oral theophylline off prescription chart
- If any life-threatening features present (see above), transfer to CCU
- refer to respiratory physician
- En-route to CCU, ensure patient accompanied by a doctor (usually an anaesthetist) prepared to intubate
MONITORING TREATMENT
- Repeat measurement of PEF 15-30 min after starting treatment then according to response
- Oximetry: maintain SpO2 94-98%
- Record heart rate and respiratory rate
- Repeat blood gas measurements within 2 hr of starting treatment if:
- initial PaO2 <8 kPa (60 mmHg), unless subsequent SpO2 >92%, or
- initial PaCO2 normal or raised, or
- patient deteriorates
- In patients requiring frequent doses of salbutamol nebuliser, repeat serum potassium within 2 hr of starting treatment and repeat 2-hrly
- potentially serious hypokalaemia especially likely to occur in patients taking corticosteroids, theophylline and diuretics, and who are hypoxic
- For monitoring of aminophylline infusion see Aminophylline guideline
- Chart PEF before and 15-20 min after giving nebulised or inhaled salbutamol
- at least four times daily until stable;
- then change to morning and evening before salbutamol dose
DISCHARGE AND FOLLOW-UP
- Carefully assess reasons for asthma attack to provide a personal asthma plan to prevent relapse, optimise treatment, and prevent delay in seeking assistance in future
- Check inhaler technique
Requirements for discharge
- Stable taking discharge medication for 24 hr and have had inhaler technique checked and recorded
- PEF >75% of predicted or best and PEF diurnal variability <25% unless discharge agreed with respiratory physician
- Treatment with oral corticosteroids for ≥7 days or until improved
- if patient on maintenance steroid treatment, discuss tapering course of steroids with asthma team
- if not on maintenance dose and course less then 3 weeks long, can stop without tapering
- Inhaled corticosteroids in addition to bronchodilators
- Own PEF meter (prescribable) - advise patient to record PEF morning and evening before inhalers
- A written personal asthma action plan
- Had reason for exacerbation discussed
- Details of admission, discharge and potential best PEF sent to GP on discharge documentation
Follow-up
- GP follow-up within 2 days
- Make outpatient clinic follow-up with asthma team
- Complete discharge checklist at the back of the care pathway
Last reviewed: 2023-12-18